What is peptide reconstitution and why does it matter?
Reconstitution is the process of dissolving a lyophilized (freeze-dried) peptide powder into a liquid solution, typically using bacteriostatic water, so it can be accurately measured and administered. Getting this step right is essential for both safety and effectiveness.
Most research peptides arrive as a delicate freeze-dried powder (lyophilized cake) sealed in a small glass vial. In this dry form, peptides are relatively stable and can be stored for extended periods. However, they must be dissolved in a sterile liquid before they can be measured in precise doses.
Improper reconstitution can lead to peptide degradation, bacterial contamination, or inaccurate dosing. Taking the time to follow proper technique protects both the integrity of the peptide and the safety of the end user.
Equipment you will need
Before starting, gather all necessary supplies. Using proper equipment ensures sterility and accuracy.
Required equipment:
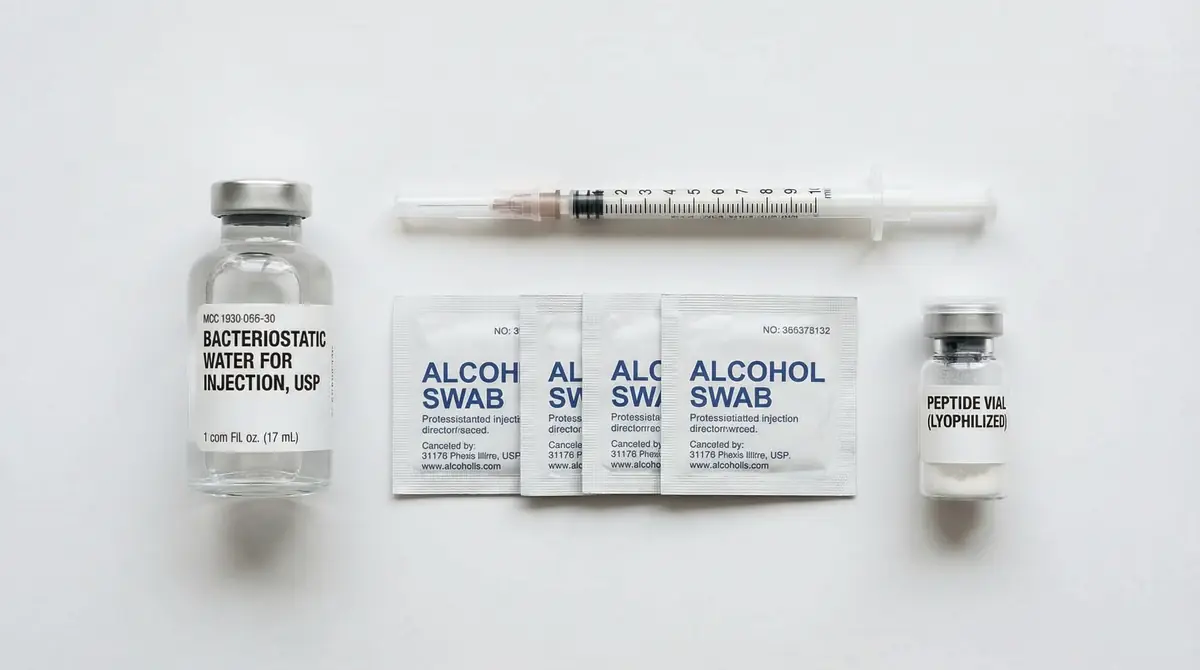
- Bacteriostatic water (BAC water): The standard reconstitution solvent. Contains 0.9% benzyl alcohol as a preservative. Available in 10mL or 30mL vials.
- Alcohol swabs (70% isopropyl): For sterilizing vial tops and injection sites.
- Insulin syringes (1mL / 100-unit): For measuring and administering the reconstituted peptide. The 100-unit markings make precise dosing easier.
- Sterile mixing syringe (1-3mL): For drawing and transferring bacteriostatic water. A larger syringe with a longer needle makes this step easier.
- Lyophilized peptide vial: Your sealed peptide in freeze-dried powder form.
Optional but recommended:
- Nitrile gloves
- Clean, flat workspace
- Sharps disposal container
Step-by-step reconstitution process
Step 1: Prepare your workspace
Clean your workspace with disinfectant. Wash your hands thoroughly and put on nitrile gloves if available. Lay out all supplies within easy reach. A clean, well-lit area reduces the risk of contamination.
Step 2: Inspect the vial
Examine the peptide vial carefully. The lyophilized powder should appear as a white or off-white cake or powder. If the powder is discolored, wet, or the vial seal is broken, do not use it. Check the expiration date if one is printed on the label.
Step 3: Swab the vial tops
Use alcohol swabs to thoroughly clean the rubber stopper on both the peptide vial and the bacteriostatic water vial. Allow the alcohol to air dry for 10-15 seconds before proceeding. This step kills surface bacteria that could contaminate the solution.
Step 4: Draw bacteriostatic water
Using the sterile mixing syringe, draw your desired amount of bacteriostatic water. Common amounts are:
| BAC water added | Result for a 5mg peptide vial |
|---|---|
| 1.0 mL | 5mg/mL (5000mcg per mL) |
| 2.0 mL | 2.5mg/mL (2500mcg per mL) |
| 2.5 mL | 2mg/mL (2000mcg per mL) |
Tip: Using 1mL or 2mL of BAC water makes the dosing math simplest.
Step 5: Add water to the peptide vial
Insert the needle through the center of the rubber stopper on the peptide vial. Do not spray the water directly onto the powder. Instead, aim the needle toward the inside wall of the vial and let the water slowly trickle down the glass wall onto the powder. This gentle approach prevents damage to the peptide’s molecular structure (2).
Step 6: Allow the peptide to dissolve
Do not shake the vial. Shaking creates turbulence that can denature (unfold) the peptide, destroying its biological activity. Instead, gently swirl the vial with a slow rotating motion, or simply place it in the refrigerator and let the powder dissolve on its own over 5-10 minutes.
The solution should become clear and colorless once fully dissolved. If particles remain after 30 minutes of gentle swirling, the peptide may be degraded.
Step 7: Store properly
Once reconstituted, immediately store the vial in the refrigerator at 2-8 degrees Celsius (36-46 degrees Fahrenheit). When stored properly with bacteriostatic water, most reconstituted peptides remain stable for 3-4 weeks.
Dosing calculations
Understanding how to calculate your dose from a reconstituted vial is critical for accuracy.
The formula:
Desired dose (mcg) divided by concentration (mcg per mL) equals volume to draw (mL).
Example: You have a 5mg BPC-157 vial reconstituted with 2mL of BAC water. You want a 250mcg dose.
- Concentration: 5000mcg / 2mL = 2500mcg per mL
- Volume needed: 250mcg / 2500mcg per mL = 0.1mL
- On a 100-unit insulin syringe, 0.1mL = 10 units (IU marks)
Common conversion: 1mL = 100 units on a standard insulin syringe.
Common mistakes to avoid
- Shaking the vial — This denatures the peptide. Always swirl gently.
- Spraying water directly onto the powder — Aim for the vial wall and let water trickle down.
- Using non-sterile water — Only use bacteriostatic water or sterile water for injection. Tap water or distilled water is not sterile.
- Skipping alcohol swabs — Every time you insert a needle through a rubber stopper, clean it with alcohol first.
- Storing at room temperature — Reconstituted peptides degrade rapidly without refrigeration.
- Reusing syringes — Use a fresh syringe for each administration to prevent contamination.
Key takeaways
- Reconstitution is the process of dissolving freeze-dried peptide powder in bacteriostatic water
- Bacteriostatic water is preferred over sterile water because its preservative allows multi-use over weeks
- Never shake peptide vials — gentle swirling or passive dissolution protects peptide integrity
- Aim water at the vial wall, not directly on the powder
- Store reconstituted peptides in the refrigerator at 2-8 degrees Celsius
- Use simple math to calculate precise doses from your reconstituted concentration
- Maintain sterility throughout the process with alcohol swabs and clean technique